Latest updates on country situation
24 June 2025
The number of malaria cases in Zimbabwe surged to 111,998 from weeks 1–23 of 2025, compared to 29,085 cases in the same period in 2024. Deaths also increased from 51 to 317, placing 67.5% of the population at risk of infection. The increase is attributed to heightened rainfall, outdoor activities, and delayed treatment. It disproportionately affected rural communities in Manicaland, Mashonaland Central, and Mashonaland West provinces. (allAfrica 24/06/2025, New Zimbabwe 24/06/2025, ZimNow 05/06/2025)
01 October 2024
In 2024, Zimbabwe is facing one of its worst droughts in 50 years as a result of El Niño. 7.6 million people are projected to face food insecurity when the current lean season peaks in February 2025. This figure is double the amount during the same period in 2024. At least three million children (60%) out of 4.9 million rely on school feeding programmes, which have encountered logistical problems and a lack of resources. The drought is also preventing 22.3% of school-age children from attending school, and malnutrition rates have risen to 4.1% in 2023 and 4.9% in 2024. Urgent action is necessary to address protection risks; provide food, WASH, education, and nutritional needs; and ensure the health of affected children. (WFP 16/09/2024, UNICEF 11/09/2024, NewsDay 01/10/2024)
24 September 2024
In 2024, southern Africa is experiencing its worst drought in 100 years as a result of El Niño. Approximately 61 million people need assistance, with over 20 million experiencing Crisis (IPC Phase 3) food insecurity levels. Botswana, Lesotho, Malawi, Namibia, Zambia, and Zimbabwe have declared a state of emergency in response to the severe drought. There has also been a significant increase in malnutrition cases in Angola, Madagascar, Malawi, Mozambique, and Zambia, with expectations for the trend to continue into the first quarter of 2025. (OCHA 20/09/2024, OCHA 19/09/2024)
30 January 2024
From December 2023 to January 2024, Zimbabwe’s inflation rose from an annual rate of 26.5% to 34.8%, while consumer prices rose by 6.6% from 4.7%. Since September 2023, consumer prices have been rising steadily, and the Zimbabwean dollar has lost about 40% of its value as at January 2024. (RZB accessed 01/02/2024, Bloomberg 29/01/2024, BT 01/02/2024)
24 October 2023
The annual consumer inflation rate in Zimbabwe fell to 18.4% in September 2023 from 77.2% in August given a change in the methodology used by the statistics agency to reflect the increased use of the US dollar in the economy, which as at August 2023 accounted for 80% of all transactions. In September, consumer prices rose by 1% compared to the previous month, and food inflation increased from 17.9% to 23.1%. (WFP 30/09/2023, TE accessed 22/10/2023)
20 September 2023
In Zimbabwe, concerns about food insecurity stemming from environmental conditions are leading more people to adopt crop diversification, water harvesting, the use of drought-tolerant crops, and consumption-based coping as the lean season approaches. The El Niño phenomenon is expected to reduce rainfall throughout the country, particularly in western areas, from October–December 2023. (WFP 31/08/2023, C3S accessed 27/09/2023)
17 July 2023
The initial effects of El Niño are leading to drier-than-normal conditions in Zimbabwe, most likely affecting food security in the coming months. The November 2023 to March 2024 period is expected to be drier than average and will coincide with the agricultural season, which might significantly affect crop planting, growth, and harvest. In 2023, an estimated three million people will be in need of humanitarian assistance, including two million children, as a result of the combined impact of climate change and the protracted economic crisis in the country. Since February 2023, a cholera outbreak has also been affecting most regions. Main needs include nutrition, health, protection, education, and WASH services. (FAO 17/07/2023, UNICEF 05/06/2023)
Analysis products
on
Zimbabwe
22 December 2022
Ripple effects of the conflict in Ukraine: truths and myths
DOCUMENT / PDF / 4 MB
This report provides a commentary on relevant datasets as it examines trends related to the economic effects of the 2022 Russian invasion of Ukraine on selected countries in the Middle East, Africa, and Asia.
29 March 2019
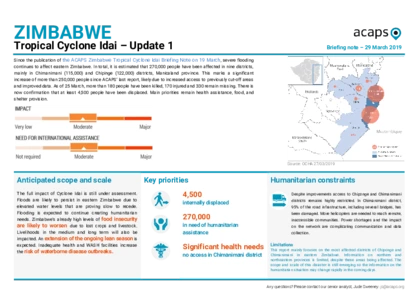
Zimbabwe: Tropical Cyclone Idai, Update I
DOCUMENT / PDF / 406 KB
Since 19 March, severe flooding continues to affect eastern Zimbabwe. In total, it is estimated that 270,000 people have been affected in nine districts, mainly in Chimanimani and Chipinge districts, Manicaland province. This marks a significant increase of more than 250,000 people since our last report.
19 March 2019
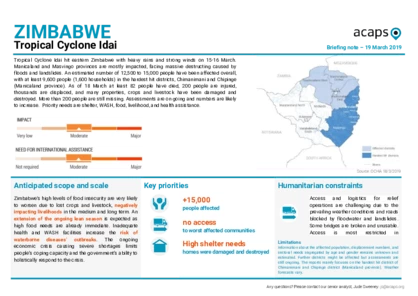
Zimbabwe: Tropical Cyclone Idai
DOCUMENT / PDF / 503 KB
Tropical Cyclone Idai hit eastern Zimbabwe with heavy rains and strong winds on 15-16 March. Manicaland and Masvingo provinces are mostly impacted, facing massive destructing caused by floods and landslides. An estimated number of 12,500 to 15,000 people have been affected overall, with at least 9,600 people in the hardest hit districts.
18 September 2018
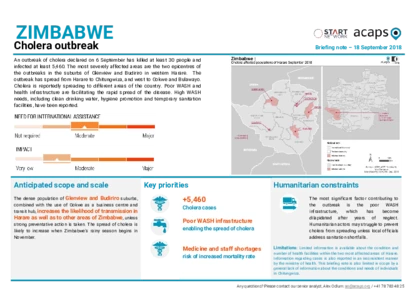
Zimbabwe: Cholera outbreak
DOCUMENT / PDF / 424 KB
An outbreak of cholera declared on 6 September has killed at least 30 people and infected at least 5,460. The most severely affected areas are the two epicentres of the outbreaks in the suburbs of Glenview and Budiriro in western Harare. The outbreak has spread from Harare to Chitungwiza, and west to Gokwe and Bulawayo.